HIPAA, PHI Management and Audit Logs Explained


Building AI systems in healthcare is not just a technical challenge. It is legal.
In many industries, data pipelines focus on:
- Scalability
- Working
- Costs
In US health care, everything revolves around:
- Compatibility
- Privacy
- Traceability
If your AI pipeline is mishandling patient data, it’s not just a bug, it’s a legitimate risk.
This is where it is ADLC (AI-driven software development lifecycle) it becomes serious. It ensures that compliance, security, and auditing are built into the system, not added later.


Basic Understanding: HIPAA and PHI
What is HIPAA?
The Health Insurance Portability and Accountability Act is the primary US law governing the protection of patient data.
It describes how healthcare data should be:
HIPAA applies to:
- Health care providers
- Insurance companies
- Health technology platforms
What is Protected Health Information (PHI)?
PHI includes any data that can identify a patient, such as:
- Names
- Addresses
- Medical records
- Lab results
- Device identifiers
Even incomplete data can qualify as PHI if it can be linked back to an individual.
Why AI Data Pipelines Are at High Risk in Healthcare
AI pipelines typically:
- Import large data sets
- Transform and enrich the data
- Feeds for predictive models
In healthcare, this creates risks such as:
- Unauthorized access
- Data leakage
- Lack of traceability
Without proper design, AI systems can easily violate HIPAA.
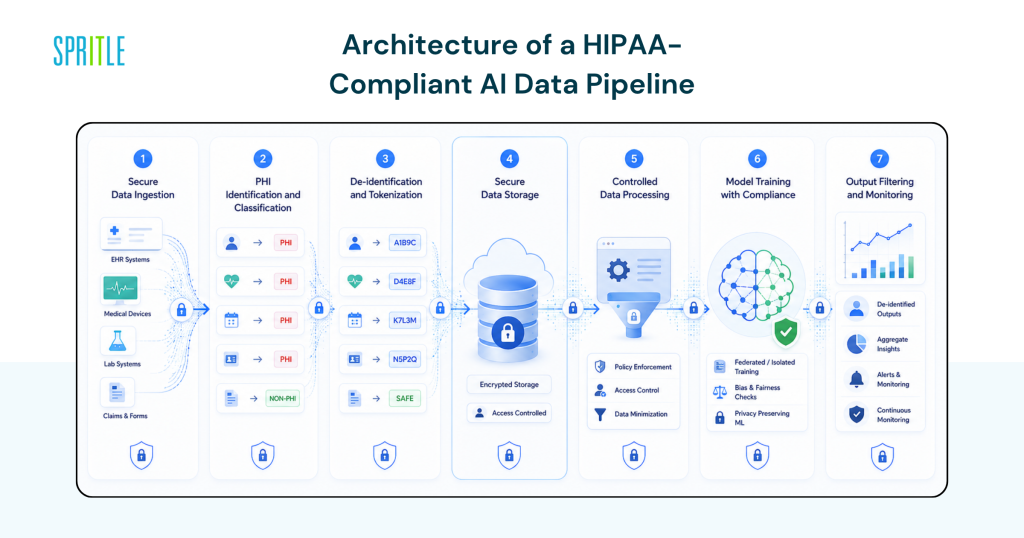
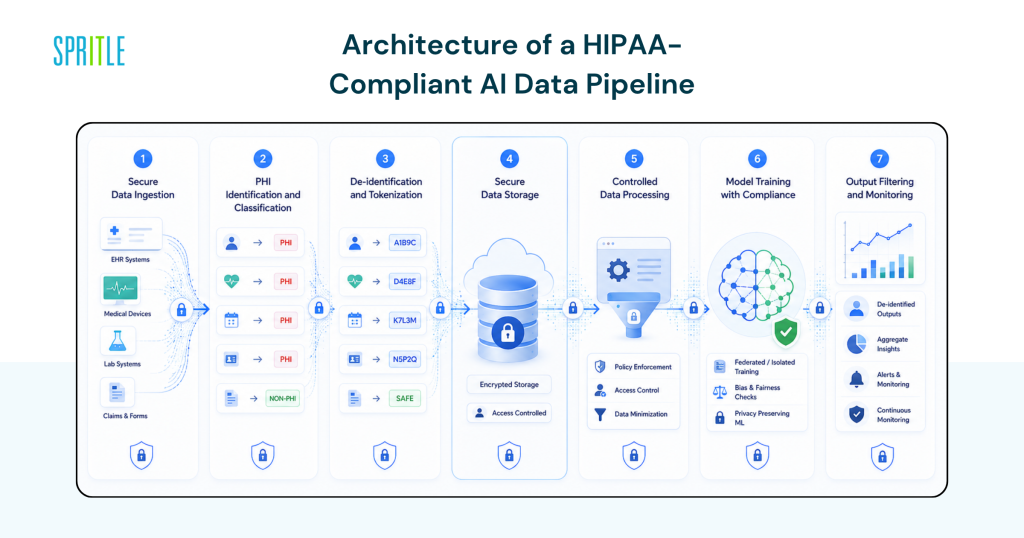
Architecture for a HIPAA-Compliant AI Data Pipeline
A compliant pipeline isn’t just about encryption—it’s about ultimate control.
1. Secure Data Entry
Data enters the system from:
- EHR systems
- APIs
- Medical devices
Best practices:
- Use encrypted channels (TLS)
- Validate data sources
- Enter strong authentication
2. PHI Identification and Classification
Before processing:
- Get PHI fields automatically
- Mark sensitive data
AI pipelines should include:
- Data classification layers
- Schema validation
3. De-identification and Tokenization
To safely use AI data:
- De-identification
- Replace with tokens (token)
This confirms:
- Models do not directly access PHI
- The data is always used for training
4. Secure Data Storage
HIPAA requires:
- Encryption at rest
- Access control methods
Use:
- Role-based Access Control (RBAC)
- Attribute-based Access Control (ABAC)
5. Data Control
During the transition:
- Minimize exposure of PHI
- Use secure computer environments
Examples:
- Independent processing containers
- Encrypted memory management
6. Model Training and Compliance
AI models should:
- Avoid memorizing PHI
- Use anonymized data sets
Techniques:
- Different privacy
- Integrated learning
7. Output Filtering and Monitoring
Before displaying the results:
- Ensure that there is no PHI leakage at the outlet
- Confirm the answers
This is especially important for:
- AI assistants
- Clinical decision tools
Audit Logs: The Core of Compliance
What are Test Logs?
Audit logs track:
- Who has access to the data
- When it is reached
- What actions are taken
They are mandatory under HIPAA.
What Should Be Included?
All pipelines must record:
- Data access events
- Data manipulation
- Verification efforts
- System errors


Key Features of a Health Audit
1. Not changing
Logs should be:
2. Granularity
Download:
- User-level actions
- Changes at the field level
3. Real Time Monitoring
Get:
- Suspicious activity
- Unauthorized access
An example of a test flow
- The doctor accesses the patient’s record
- System logs:
- User ID
- Time stamp
- Data has been accessed
- The AI model processes anonymous data
- The output has been entered and verified
This ensures full traceability.
How ADLC Ensures Design Compliance
Traditional pipes:
ADLC pipelines:
- Build consistency across all categories
Continuous Compliance Monitoring
- Automatic policy validation
- Real-time alerts
AI Lifecycle Governance
- Track the data list
- Monitor the behavior model
AutoText
- Generate compliance reports
- Make it easy to test
Common Mistakes in Healthcare AI Pipelines
Storing raw PHI in training data
Risks:
- Data leakage
- Violation of the law
Weak Access Controls
Risks:
Lost Test Methods
Risks:
Forward Discharge Leakage
AI responses may:
Best Practices for Building Secure Pipelines
Minimize Use of PHI
Collect only:
- What is absolutely necessary
Nail It All
- Data in transport
- The data is at rest
Use Zero Trust Architecture
- Verify all access requests
- There is no direct trust
Regular Audits and Inspections
- Conduct compliance checks
- Simulate attack scenarios
Real World Applications
Clinical Decision Support Systems
AI analyzes:
- Patient history
- Lab results
While verifying:
Remote Patient Monitoring
Sending devices:
The pipeline ensures:
- Secure import
- Continuous monitoring
Chatbots for Healthcare
AI interacts with patients:
- He answers the questions
- It provides guidance
You must confirm:
- No leakage of PHI in responses
FAQ
Q: What is PHI in AI pipelines?
A: PHI is any data that identifies a patient that must be protected under HIPAA during collection, processing, and storage.
Q: How do audit logs help with compliance?
A: Provides traceability of all data access and actions, required for HIPAA audits and security monitoring.
Q: Can AI models be trained on PHI?
A: Yes, but only with strong protections such as anonymity, consent, and protected areas.
Q: What is ADLC’s role in AI healthcare?
A: ADLC ensures compliance, security, and governance are integrated at all stages of the AI pipeline.
The conclusion
AI in healthcare is powerful—but also highly regulated.
To build reliable systems, teams must go beyond functionality and focus on:
- Compatibility
- Data protection
- Auditability
By combining these in The AI-driven software development life cycleorganizations can build AI pipelines that are not only intelligent—but also secure, compliant, and reliable.
In health care, that is not an option. It is important.